Business Name: BeeHive Homes Assisted Living
Address: 16220 West Rd, Houston, TX 77095
Phone: (832) 906-6460
BeeHive Homes Assisted Living
BeeHive Homes Assisted Living of Cypress offers assisted living and memory care services in a warm, comfortable, and residential setting. Our care philosophy focuses on personalized support, safety, dignity, and building meaningful connections for each resident. Welcoming new residents from the Cypress and surrounding Houston TX community.
16220 West Rd, Houston, TX 77095
Business Hours
Monday thru Sunday: 7:00am - 7:00pm
Facebook: https://www.facebook.com/BeeHiveHomesCypress
Families usually concern memory care after months, often years, of managing little changes that grow into huge risks: a stove left on, a fall in the evening, the sudden anxiety of not recognizing a familiar hallway. Good dementia care does not begin with technology or architecture. It starts with regard for a person's rhythm, choices, and self-respect, then utilizes thoughtful style and practice to keep that individual engaged and safe. The best assisted living communities that focus on memory care keep this at the center of every decision, from door hardware to everyday schedules.
The last years has actually brought constant, practical improvements that can make daily life calmer and more significant for residents. Some are subtle, the angle of a hand rails that dissuades leaning, or the color of a bathroom flooring that reduces bad moves. Others are programmatic, such as brief, regular activity blocks instead of long group sessions, or meal menus that adjust to altering motor capabilities. A number of these ideas are simple to adopt at home, which matters for households utilizing respite care or supporting a loved one in between check outs. What follows is a close take a look at what works, where it assists most, and how to weigh alternatives in senior living.
Safety by Design, Not by Restraint
A safe environment does not have to feel locked down. The very first objective is to reduce the opportunity of damage without eliminating freedom. That begins with the floor plan. Short, looping passages with visual landmarks assist a resident find the dining-room the very same way every day. Dead ends raise frustration. Loops lower it. In small-house designs, where 10 to 16 homeowners share a typical area and open kitchen area, personnel can see more of the environment at a glance, and locals tend to mirror one another's regimens, which supports the day.
Lighting is the next lever. Older eyes need more light, and dementia magnifies level of sensitivity to glare and shadow. Overhead fixtures that spread even, warm lighting cut down on the "great void" impression that dark doorways can create. Motion-activated path lights assist at night, especially in the 3 hours after midnight when numerous residents wake to utilize the bathroom. In one building I worked with, replacing cool blue lights with 2700 to 3000 Kelvin bulbs and adding continuous under-cabinet lighting in the cooking area reduced nighttime falls by a 3rd over 6 months. That was not a randomized trial, however it matched what personnel had observed for years.
Color and contrast matter more than style publications suggest. A white toilet on a white flooring can vanish for someone with depth understanding modifications. A sluggish, non-slip, mid-tone flooring, a plainly contrasted toilet seat, and a solid shower chair boost confidence. Avoid patterned floorings that can appear like obstacles, and avoid shiny finishes that mirror like puddles. The goal is to make the appropriate option apparent, not to force it.
Door choices are another peaceful innovation. Rather than hiding exits, some neighborhoods redirect attention with murals or a resident's memory box positioned close by. A memory box, the size of a shadow frame, holds individual items and photographs that cue identity and orient somebody to their space. It is not decor. It is a lighthouse. Basic door hardware, lever instead of knob, helps arthritic hands. Delaying unlocking with a quick, staff-controlled time lock can provide a team enough time to engage a person who wishes to stroll outside without developing the sensation of being trapped.
Finally, believe in gradients of security. A totally open courtyard with smooth walking courses, shaded benches, and waist-high plant beds welcomes movement without the dangers of a parking lot or city pathway. Add sightlines for personnel, a couple of gates that are staff-keyed, and a paved loop wide enough for two walkers side by side. Movement diffuses agitation. It likewise maintains muscle tone, hunger, and mood.
Calming the Day: Rhythms, Not Rigid Schedules
Dementia impacts attention span and tolerance for overstimulation. The very best daily strategies regard that. Instead of 2 long group activities, think in blocks of 15 to 40 minutes that flow from one to the next. A morning may begin with coffee and music at private tables, shift to a brief, assisted stretch, then a choice in between a folding laundry station or an art table. These are not busywork. They recognize jobs with a function that aligns with past roles.
A resident who worked in a workplace may settle with a basket of envelopes to sort and stamps to location. A previous carpenter may sand a soft block of wood or assemble safe PVC pipe puzzles. Someone who raised kids may pair child clothes or arrange little toys. When these choices reflect an individual's history, participation increases, and agitation drops.
Meal timing is another rhythm lever. Cravings changes with disease stage. Providing 2 lighter breakfasts, separated by an hour, can increase overall consumption without forcing a large plate at the same time. Finger foods get rid of the barrier of utensils when tremblings or motor planning make them frustrating. A turkey and cranberry slider can deliver the very same nutrition as a plated roast when cut correctly. Foods with color contrast are simpler to see, so blueberries in oatmeal or a slice of tomato beside an egg boosts both appeal and independence.
Sundowning, the late afternoon swell of confusion or anxiety, deserves its own strategy. Dimmer spaces, loud televisions, and loud corridors make it worse. Personnel can preempt it by moving to tactile activities in brighter, calmer spaces around 3 p.m., and by timing a snack with protein and hydration around the very same hour. Families often help by visiting sometimes that fit the resident's energy, not the family's benefit. A 20-minute visit at 10 a.m. for an early morning person is better than a 60-minute visit at 5 p.m. that activates a meltdown.
Technology That Quietly Helps
Not every gizmo belongs in memory care. The bar is high: it should lower threat or increase quality of life without adding a layer of confusion. A couple of classifications pass the test.
Passive movement sensors and bed exit pads can inform personnel when someone gets up in the evening. The very best systems discover patterns over time, so they do not alarm each time a resident shifts. Some neighborhoods connect restroom door sensing units to a soft light hint and a staff notice after a timed period. The point is not to race in, however to examine if a resident needs help dressing or is disoriented.
Wearable gadgets have blended outcomes. Action counters and fall detectors help active citizens happy to use them, particularly early beehivehomes.com assisted living in the disease. Later on, the device becomes a foreign item and might be gotten rid of or fiddled with. Area badges clipped discreetly to clothes are quieter. Privacy issues are real. Families and neighborhoods should settle on how data is used and who sees it, then review that contract as requirements change.
Voice assistants can be useful if placed smartly and set up with strict personal privacy controls. In personal rooms, a device that responds to "play Ella Fitzgerald" or "what time is supper" can lower recurring questions to personnel and ease solitude. In common locations, they are less effective since cross-talk confuses commands. The increase of wise induction cooktops in presentation kitchen areas has likewise made cooking programs more secure. Even in assisted living, where some residents do not need memory care, induction cuts burn threat while allowing the happiness of preparing something together.

The most underrated innovation stays environmental control. Smart thermostats that prevent huge swings in temperature level, motorized blinds that keep glare consistent, and lighting systems that shift color temperature across the day support circadian rhythm. Staff see the distinction around 9 a.m. and 7 p.m., when locals settle more quickly. None of this replaces human attention. It extends it.
Training That Sticks
All the style worldwide fails without competent individuals. Training in memory care need to exceed the disease fundamentals. Personnel require useful language tools and de-escalation techniques they can utilize under tension, with a focus on in-the-moment issue solving. A couple of concepts make a trustworthy backbone.
Approach counts more than content. Standing to the side, moving at the resident's speed, and offering a single, concrete cue beats a flurry of directions. "Let's try this sleeve initially" while gently tapping the best forearm accomplishes more than "Put your t-shirt on." If a resident refuses, circling back in five minutes after resetting the scene works better than pressing. Aggression frequently drops when personnel stop trying to argue facts and rather verify sensations. "You miss your mother. Inform me her name," opens a course that "Your mother passed away 30 years ago" shuts.
Good training utilizes role-play and feedback. In one neighborhood, brand-new hires practiced rerouting a colleague posing as a resident who wished to "go to work." The best responses echoed the resident's career and rerouted toward a related job. For a retired instructor, staff would state, "Let's get your classroom all set," then stroll towards the activity room where books and pencils were waiting. That type of practice, duplicated and strengthened, develops into muscle memory.
Trainees likewise need assistance in principles. Balancing autonomy with safety is not easy. Some days, letting somebody walk the yard alone makes good sense. Other days, tiredness or heat makes it a bad option. Staff should feel comfy raising the trade-offs, not simply following blanket rules, and supervisors need to back judgment when it includes clear thinking. The outcome is a culture where residents are dealt with as adults, not as tasks.
Engagement That Means Something
Activities that stick tend to share 3 characteristics: they recognize, they utilize multiple senses, and they offer a chance to contribute. It is tempting to fill a calendar with events that look great in photos. Households delight in seeing a smiling group in matching hats, and every so often a party does lift everybody. Daily engagement, though, often looks quieter.
Music is a trusted anchor. Personalized playlists, built from a resident's teens and twenties, tap into maintained memory pathways. A headphone session of 10 minutes before bathing can alter the whole experience. Group singing works best when song sheets are unneeded and the songs are deeply known. Hymns, folk requirements, or regional favorites carry more power than pop hits, even if the latter feel present to staff.
Food, managed securely, offers endless entry points. Shelling peas, kneading dough, slicing soft fruit with a safe knife, or rolling meatballs links hands and nose to memory. The fragrance of onions in butter is a stronger cue than any poster. For citizens with innovative dementia, just holding a warm mug and breathing in can soothe.
Outdoor time is medication. Even a small patio transforms state of mind when utilized regularly. Seasonal rituals help, planting herbs in spring, harvesting tomatoes in summertime, raking leaves in fall. A resident who lived his entire life in the city may still enjoy filling a bird feeder. These acts validate, I am still required. The feeling lasts longer than the action.
Spiritual care extends beyond official services. A peaceful corner with a scripture book, prayer beads, or a basic candle for reflection aspects varied customs. Some citizens who no longer speak completely sentences will still whisper familiar prayers. Personnel can find out the basics of a few traditions represented in the community and cue them respectfully. For residents without religious practice, secular rituals, reading a poem at the very same time each day, or listening to a specific piece of music, supply similar structure.
Measuring What Matters
Families often request numbers. They deserve them. Falls, weight changes, medical facility transfers, and psychotropic medication usage are standard metrics. Communities can include a couple of qualitative steps that reveal more about lifestyle. Time spent outdoors per resident weekly is one. Frequency of meaningful engagement, tracked simply as yes or no per shift with a short note, is another. The goal is not to pad a report, however to assist attention. If afternoon agitation rises, recall at the week's light direct exposure, hydration, and staff ratios at that hour. Patterns emerge quickly.

Resident and household interviews include depth. Ask families, did you see your mother doing something she loved today? Ask locals, even with minimal language, what made them smile today. When the answer is "my child checked out" 3 days in a row, that tells you to arrange future interactions around that anchor.
Medications, Habits, and the Middle Path
The severe edge of dementia shows up in behaviors that frighten families: yelling, getting, sleep deprived nights. Medications can assist in particular cases, however they bring dangers, specifically for older adults. Antipsychotics, for example, increase stroke threat and can dull quality of life. A mindful process starts with detection and paperwork, then ecological adjustment, then non-drug approaches, then targeted, time-limited medication trials with clear objectives and regular reassessment.
Staff who know a resident's standard can typically spot triggers. Loud commercials, a certain staff approach, pain, urinary system infections, or irregularity lead the list. An easy pain scale, adjusted for non-verbal indications, catches lots of episodes that would otherwise be identified "resistance." Treating the discomfort eases the behavior. When medications are used, low dosages and specified stop points minimize the possibility of long-lasting overuse. Households must expect both sincerity and restraint from any senior living provider about psychotropic prescribing.
Assisted Living, Memory Care, and When to Pick Respite
Not everyone with dementia needs a locked unit. Some assisted living neighborhoods can support early-stage residents well with cueing, house cleaning, and meals. As the illness progresses, specialized memory care adds value through its environment and staff know-how. The trade-off is typically cost and the degree of flexibility of movement. An honest evaluation looks at safety incidents, caregiver burnout, roaming danger, and the resident's engagement in the day.
Respite care is the overlooked tool in this series. A planned stay of a week to a month can stabilize regimens, provide medical tracking if needed, and provide household caregivers real rest. Great communities utilize respite as a trial period, introducing the resident to the rhythms of memory care without the pressure of a permanent move. Households discover, too, observing how their loved one reacts to group dining, structured activities, and different sleeping patterns. An effective respite stay typically clarifies the next step, and when a return home makes good sense, personnel can recommend ecological tweaks to bring forward.
Family as Partners, Not Visitors
The finest outcomes occur when households remain rooted in the care strategy. Early on, families can fill a "life story" document with more than generalities. Specifics matter. Not "loved music," however "sang alto in the Bethany choir, 1962 to 1970." Not "worked in financing," but "bookkeeper who balanced the ledger by hand every Friday." These details power engagement and de-escalation.
Visiting patterns work much better when they fit the person's energy and lower transitions. Call or video chats can be brief and regular rather than long and rare. Bring items that connect to previous roles, a bag of sorted coins to roll, dish cards in familiar handwriting, a baseball radio tuned to the home team. If a visit raises agitation, shorten it and move the time, instead of pressing through. Personnel can coach households on body movement, using less words, and using one option at a time.
Grief is worthy of a place in the partnership. Families are losing parts of an individual they enjoy while also handling logistics. Neighborhoods that acknowledge this, with month-to-month support groups or individually check-ins, foster trust. Basic touches, a staff member texting a picture of a resident smiling throughout an activity, keep families connected without varnish.
The Little Developments That Include Up
A few practical modifications I have actually seen settle across settings:
- Two clocks per room, one analog with dark hands on a white face, one digital with the day and date spelled out, decrease repeated "what time is it" questions and orient homeowners who check out much better than they calculate. A "busy box" kept by the front desk with headscarfs to fold, old postcards to sort, a deck of large-print cards, and a soft brush for easy grooming jobs uses instant redirection for somebody anxious to leave. Weighted lap blankets in common spaces lower fidgeting and offer deep pressure that calms, particularly throughout movies or music sessions. Soft, color-coded tableware, red for lots of homeowners, increases food intake by making parts noticeable and plates less slippery. Staff name tags with a big given name and a single word about a hobby, "Maria, baking," humanize interactions and stimulate conversation.
None of these needs a grant or a remodel. They need attention to how individuals really move through a day.
Designing for Self-respect at Every Stage
Advanced dementia challenges every system. Language thins, movement fades, and swallowing can falter. Self-respect stays. Spaces must adapt with hospital-grade beds that look residential, not institutional. Ceiling raises spare backs and bruised arms. Bathing shifts to a warmth-first approach, with towels preheated and the room established before the resident enters. Meals highlight satisfaction and security, with textures changed and flavors protected. A puréed peach served in a little glass bowl with a sprig of mint checks out as food, not as medicine.
End-of-life care in memory systems take advantage of hospice collaborations. Integrated teams can treat pain strongly and support families at the bedside. Staff who have understood a resident for several years are frequently the very best interpreters of subtle cues in the last days. Routines assist here, too, a quiet song after a death, a note on the community board honoring the individual's life, consent for personnel to grieve.
Cost, Access, and the Realities Households Face
Innovations do not eliminate the fact that memory care is pricey. In lots of regions of the United States, private-pay rates range from the mid 4 figures to well above 10 thousand dollars each month, depending on care level and place. Medicare does not cover room and board in assisted living or memory care. Medicaid waivers can help in some states, however slots are restricted and waitlists long. Long-term care insurance can balance out expenses if bought years earlier. For households drifting in between options, combining adult day programs with home care can bridge time till a relocation is required. Respite stays can likewise stretch capacity without devoting prematurely to a complete transition.
When touring neighborhoods, ask specific questions. How many residents per team member on day and night shifts? How are call lights kept an eye on and escalated? What is the fall rate over the past quarter? How are psychotropic medications reviewed and reduced? Can you see the outside space and enjoy a mealtime? Unclear responses are an indication to keep looking.
What Development Looks Like
The finest memory care communities today feel less like wards and more like communities. You hear music tuned to taste, not a radio station left on in the background. You see residents moving with function, not parked around a tv. Personnel usage first names and gentle humor. The environment pushes rather than dictates. Family photos are not staged, they are lived in.
Progress can be found in increments. A restroom that is easy to browse. A schedule that matches a person's energy. An employee who understands a resident's college fight tune. These information amount to security and delight. That is the genuine development in memory care, a thousand small options that honor an individual's story while fulfilling today with skill.
For households searching within senior living, including assisted living with devoted memory care, the signal to trust is simple: enjoy how the people in the room take a look at your loved one. If you see perseverance, interest, and respect, you have most likely discovered a place where the innovations that matter a lot of are currently at work.
BeeHive Homes Assisted Living is an Assisted Living Facility
BeeHive Homes Assisted Living is an Assisted Living Home
BeeHive Homes Assisted Living is located in Cypress, Texas
BeeHive Homes Assisted Living is located Northwest Houston, Texas
BeeHive Homes Assisted Living offers Memory Care Services
BeeHive Homes Assisted Living offers Respite Care (short-term stays)
BeeHive Homes Assisted Living provides Private Bedrooms with Private Bathrooms for their senior residents
BeeHive Homes Assisted Living provides 24-Hour Staffing
BeeHive Homes Assisted Living serves Seniors needing Assistance with Activities of Daily Living
BeeHive Homes Assisted Living includes Home-Cooked Meals Dietitian-Approved
BeeHive Homes Assisted Living includes Daily Housekeeping & Laundry Services
BeeHive Homes Assisted Living features Private Garden and Green House
BeeHive Homes Assisted Living has a Hair/Nail Salon on-site
BeeHive Homes Assisted Living has a phone number of (832) 906-6460
BeeHive Homes Assisted Living has an address of 16220 West Road, Houston, TX 77095
BeeHive Homes Assisted Living has website https://beehivehomes.com/locations/cypress
BeeHive Homes Assisted Living has Google Maps listing https://maps.app.goo.gl/G6LUPpVYiH79GEtf8
BeeHive Homes Assisted Living has Facebook page https://www.facebook.com/BeeHiveHomesCypress
BeeHive Homes Assisted Living is part of the brand BeeHive Homes
BeeHive Homes Assisted Living focuses on Smaller, Home-Style Senior Residential Setting
BeeHive Homes Assisted Living has care philosophy of “The Next Best Place to Home”
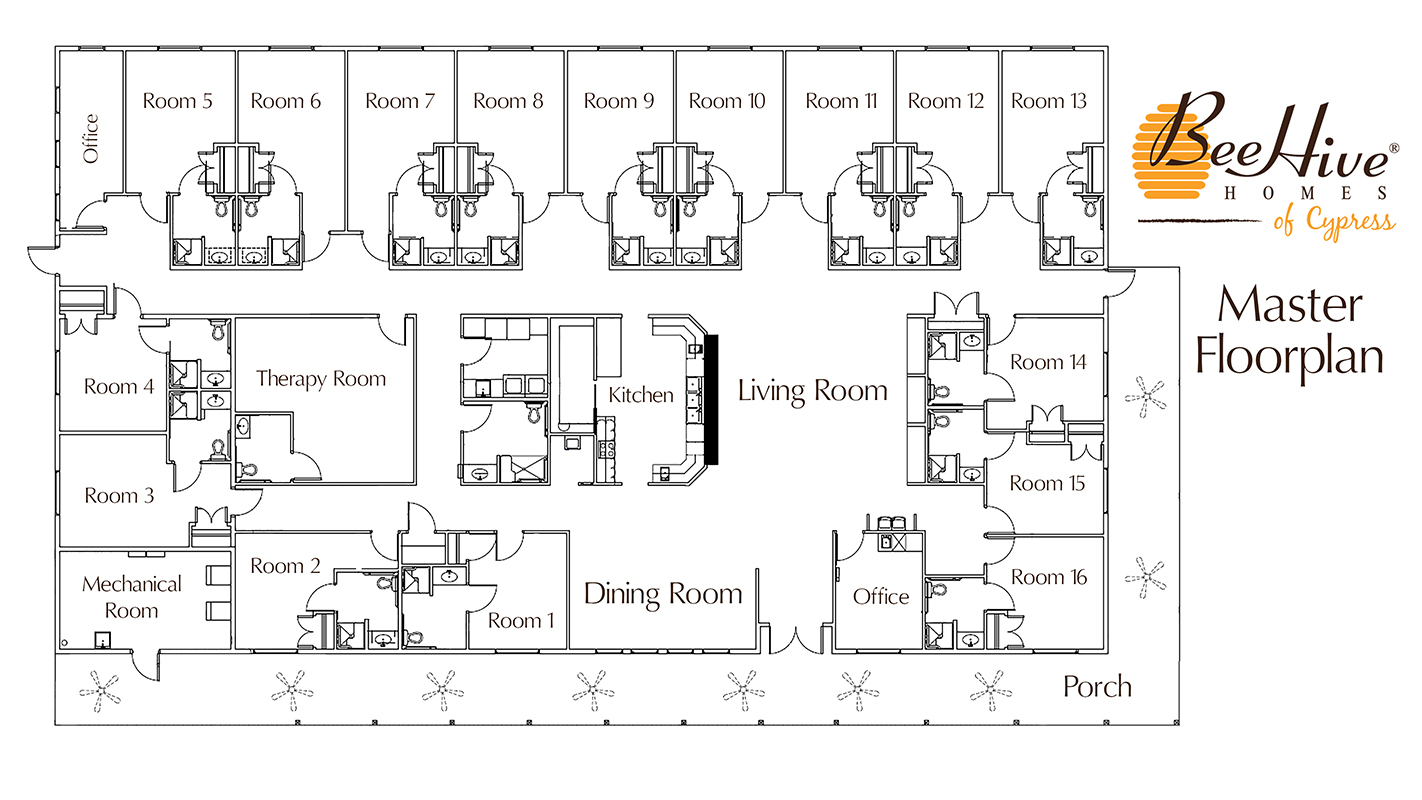
BeeHive Homes Assisted Living has floorplan of 16 Private Bedrooms with ADA-Compliant Bathrooms
BeeHive Homes Assisted Living welcomes Families for Tours & Consultations
BeeHive Homes Assisted Living promotes Engaging Activities for Senior Residents
BeeHive Homes Assisted Living emphasizes Personalized Care Plans for each Resident
BeeHive Homes Assisted Living won Top Branded Assisted Living Houston 2025
BeeHive Homes Assisted Living earned Outstanding Customer Service Award 2024
BeeHive Homes Assisted Living won Excellence in Assisted Living Homes 2023
People Also Ask about BeeHive Homes Assisted Living
What services does BeeHive Homes Assisted Living of Cypress provide?
BeeHive Homes Assisted Living of Cypress provides a full range of assisted living and memory care services tailored to the needs of seniors. Residents receive help with daily activities such as bathing, dressing, grooming, medication management, and mobility support. The community also offers home-cooked meals, housekeeping, laundry services, and engaging daily activities designed to promote social interaction and cognitive stimulation. For individuals needing specialized support, the secure memory care environment provides additional safety and supervision.
How is BeeHive Homes Assisted Living of Cypress different from larger assisted living facilities?
BeeHive Homes Assisted Living of Cypress stands out for its small-home model, offering a more intimate and personalized environment compared to larger assisted living facilities. With 16 residents, caregivers develop deeper relationships with each individual, leading to personalized attention and higher consistency of care. This residential setting feels more like a real home than a large institution, creating a warm, comfortable atmosphere that helps seniors feel safe, connected, and truly cared for.
Does BeeHive Homes Assisted Living of Cypress offer private rooms?
Yes, BeeHive Homes Assisted Living of Cypress offers private bedrooms with private or ADA-accessible bathrooms for every resident. These rooms allow individuals to maintain dignity, independence, and personal comfort while still having 24-hour access to caregiver support. Private rooms help create a calmer environment, reduce stress for residents with memory challenges, and allow families to personalize the space with familiar belongings to create a “home-within-a-home” feeling.
Where is BeeHive Homes Assisted Living located?
BeeHive Homes Assisted Living is conveniently located at 16220 West Road, Houston, TX 77095. You can easily find direction on Google Maps or visit their home during business hours, Monday through Sunday from 7am to 7pm.
How can I contact BeeHive Homes Assisted Living?
You can contact BeeHive Assisted Living by phone at: 832-906-6460, visit their website at https://beehivehomes.com/locations/cypress/, or connect on social media via Facebook
Take good care of your senior parents and then take Mom or Dad out to the movies, Cinemark Cypress and XD located near us!